They Need a Ventilator To Stay Alive. Getting One Can Be a Nightmare.
On vacation in Mexico last year, Michael DiPlacido passed out twice while scuba diving and again in his hotel. Back in St. Louis, doctors diagnosed him with amyotrophic lateral sclerosis, or ALS, an incurable disease that often requires mechanical ventilation.
When his son Adam DiPlacido tried to find a permanent place to care for his father, who now needed a ventilator to breathe through a tracheostomy tube, he discovered none of Missouri’s nearly 500 nursing homes could take him.
“I never thought it would be easy, but I never thought it would be this hard,” Adam said.
A KFF Health News investigation found widespread flaws and gaps in care for some of the country’s most debilitated people: those who cannot breathe on their own.
Spinal cord injuries, strokes, chronic obstructive pulmonary disease, and neurological diseases such as multiple sclerosis have left tens of thousands of Americans permanently dependent on ventilators. The barriers these patients face offer a stark example of how the United States’ disjointed health care system makes dealing with severe illness so much harder.
The investigation found patients are frequently stymied in efforts to get their insurers to provide appropriate home ventilators. They can end up spending hundreds of thousands of dollars for private nurses to make sure they don’t die overnight. Those who need to be in a nursing home or other health facility sometimes must move to another state, far from their families.
“There are not a lot of institutions that can manage these people,” said Jonathon Schwartz, acting chief medical officer for the Spaulding Rehabilitation Network in Boston.
Only 347 of the nation’s roughly 14,750 nursing homes have specialized units dedicated to people on ventilators, a KFF Health News analysis of federal data shows. Fifteen states, including Missouri, have no nursing homes with a specialized unit for ventilator care.
While nursing homes can care for residents on ventilators on their regular floors, in practice few do. From April through June, fewer than 10% of nursing homes had long-stay residents breathing with the assistance of invasive mechanical ventilators, which deliver air through a tube down the airway or via a tracheostomy, the analysis found. Fewer than 15% of nursing homes had short-stay patients on ventilators.
Many patients in nursing homes can be weaned off ventilators, but those who can’t because of their condition often spend years in hospitals, which are not designed for residency. Innovative alternatives to traditional nursing homes exist in some areas of the country, but they haven’t been widely replicated and now are at risk from steep reductions in Medicaid enacted by President Donald Trump and the Republican-controlled Congress.
“It could create a terrible scenario,” said Gene Gantt, a respiratory care consultant to states and insurers.
Many people permanently on ventilators prefer to live at home as long as they can. But care there can be perilous and pricey. Some state health programs pay for ventilator care for low-income patients, but getting enrolled can take months amid bureaucratic hurdles and waitlists.
Some insurers balk at providing advanced home ventilators — which sound alerts for collapsed lungs, airway leaks, or malfunctions and can cost more than $10,000 — until patients have lost much of their ability to breathe.
“Feeling you’re suffocating is a horrific feeling, and that feeling can go on for months and months” as ALS patients decline while sparring with insurers, said Tyler Rehbein, an assistant professor of neurology at the University of Rochester who treats ALS patients.
‘Out of Money’
David Goldstein’s first symptom of ALS was a limp that appeared in the fall of 2022. It took six months for doctors to diagnose him with the neuromuscular disorder, also known as Lou Gehrig’s Disease. ALS afflicts about 34,000 Americans, destroying the nerve cells in the brain and spinal cord that control muscles, including those for breathing. It eventually results in complete paralysis, while most people remain mentally alert. Patients usually end up on ventilators if they do not die first, and respiratory failure is the most common cause of death.
Now 69 and on a ventilator, David cannot move anything except his eyes and mouth, said his ex-wife, Janis Goldstein, who has power of attorney. He requires someone around all the time in his Houston apartment to feed and bathe him, give him medication, and remove mucus blocking his airway. The settings on the ventilator require frequent monitoring and adjustments.
In spring of 2023, David got on the waiting list for Texas’ Medicaid home health program for disabled adults. More than a year later, Texas authorized 12 hours of home care a day. Still, Janis said, the state’s designated administrator sometimes has trouble getting workers for those shifts, and she and her ex-husband must pay for nurses to cover the rest of the day or night.
She said they have spent around a half-million dollars, largely on nurses and aides. They raised much of it through online campaigns and a fundraiser headlined by the country singer Larry Gatlin.
“The point that we’re at now, with the 24-hour help, is we’re pretty much out of money,” Janis said.
She is planning to move David into one of the few nursing homes in the region that take patients on ventilators, she said, but is concerned it will be difficult to arrange for someone to stay with David overnight in his room. She fears that if David’s position shifts even half an inch, he won’t be able to call for help through the machine that tracks his eye movements.
“I don’t know that he’ll be able to handle the stress and the anxiety of knowing that he could suffocate, even in a facility, because he doesn’t have someone by his side,” she said.
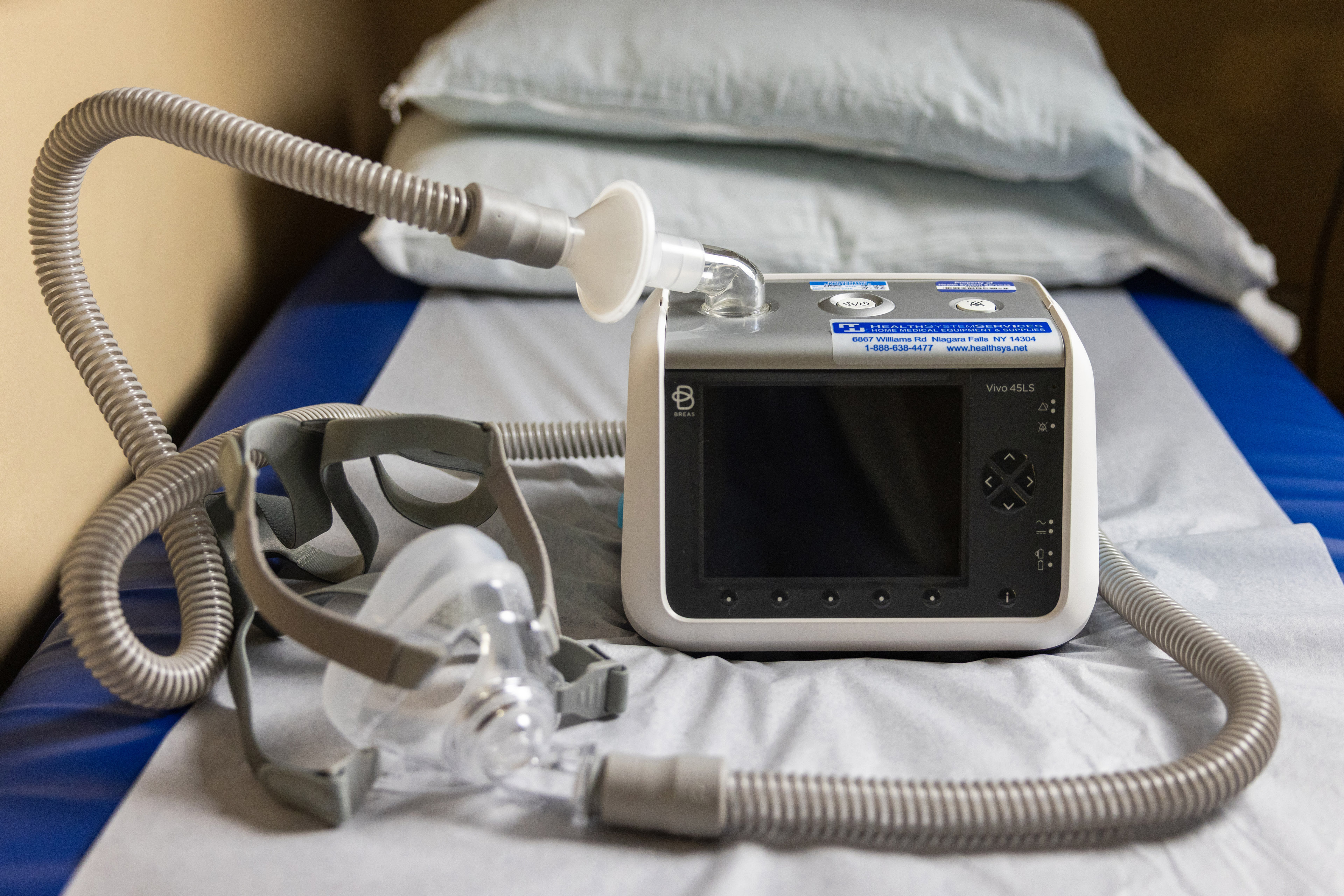
Ventilator Deserts
When Michael DiPlacido’s son Adam spent weeks searching for a facility in Missouri that could take care of a patient on a ventilator with a trach tube, the only one that was even a possibility told him it couldn’t accept new patients, because its lone respiratory therapist had quit.
“It’s incredible to me there is not one single place in Missouri that can take a patient like my father,” Adam said.
Looking outside the state, Michael decided to move to a nursing home north of Chicago, about five hours by car from St. Louis. After three months, he left the facility because it was so far away from his family, Adam said.
Adam helped his father move into a long-term care hospital in suburban St. Louis for six weeks. But Michael’s insurer would not pay for hospital-level acute care, so Adam said Michael had to pay more than $47,000 out-of-pocket. Next, Adam helped him move to another Illinois nursing home, about an hour away, that his son had originally rejected because of online reviews, including a Medicare warning that abuse had occurred. Finding it deficient, Michael left after a week.
Adam found a private nursing home company that would care for Michael in his home, at a cost of $960 a day. “After 323 days, my father has finally made it back home,” Adam said in an email in September.
But with his health rapidly deteriorating, Michael was admitted to a hospice facility in October. He died later that month at 75.

Gantt, the respiratory care consultant, said that fewer than half of state Medicaid programs provide adequate reimbursement rates for ventilator patients. He said most state Medicaid payment formulas do not measure outcomes or reward nursing homes financially if they provide better care, such as weaning a patient off the ventilator or preventing infections. He said he has seen nursing homes accept patients with trach tubes even when nurses lack proper training, or when the facility doesn’t employ respiratory therapists.
“For the large part, these patients are stuck in bed,” Gantt said. “We should try to get them the best quality of life.”
David Gifford, the chief medical officer for the American Health Care Association, a nursing home trade group, said equipping a nursing home with ventilators and getting state approval is expensive, and outside of urban areas, many markets lack enough local patients who need ventilators to make it financially worthwhile.
“It’s not as simple as saying we’re going to pay more and have more respiratory therapists,” Gifford said. “This is a group that needs highly specialized care. You’re not going to have it everywhere.”
Flagging Breaths
Derek McManus’ weakening right hand and occasional twitching was the first sign something was wrong. In October 2023, doctors diagnosed Derek, a corporate executive who lives in Painted Post, New York, with ALS.
By August 2024, Derek’s lungs were operating at 78% of capacity, his medical records show. Because ALS progresses so quickly, doctors often prescribe advanced home mechanical ventilators. These machines deliver high-pressure air through a mask (called non-invasive) or a tube down the airway or via a tracheostomy (called invasive). They can calibrate themselves based on a patient’s breathing and have alarms that detect leaks, airway blockages, and device malfunctions. They can run on portable power sources and backup batteries in case of a power failure. The machines can allow people to talk or eat.
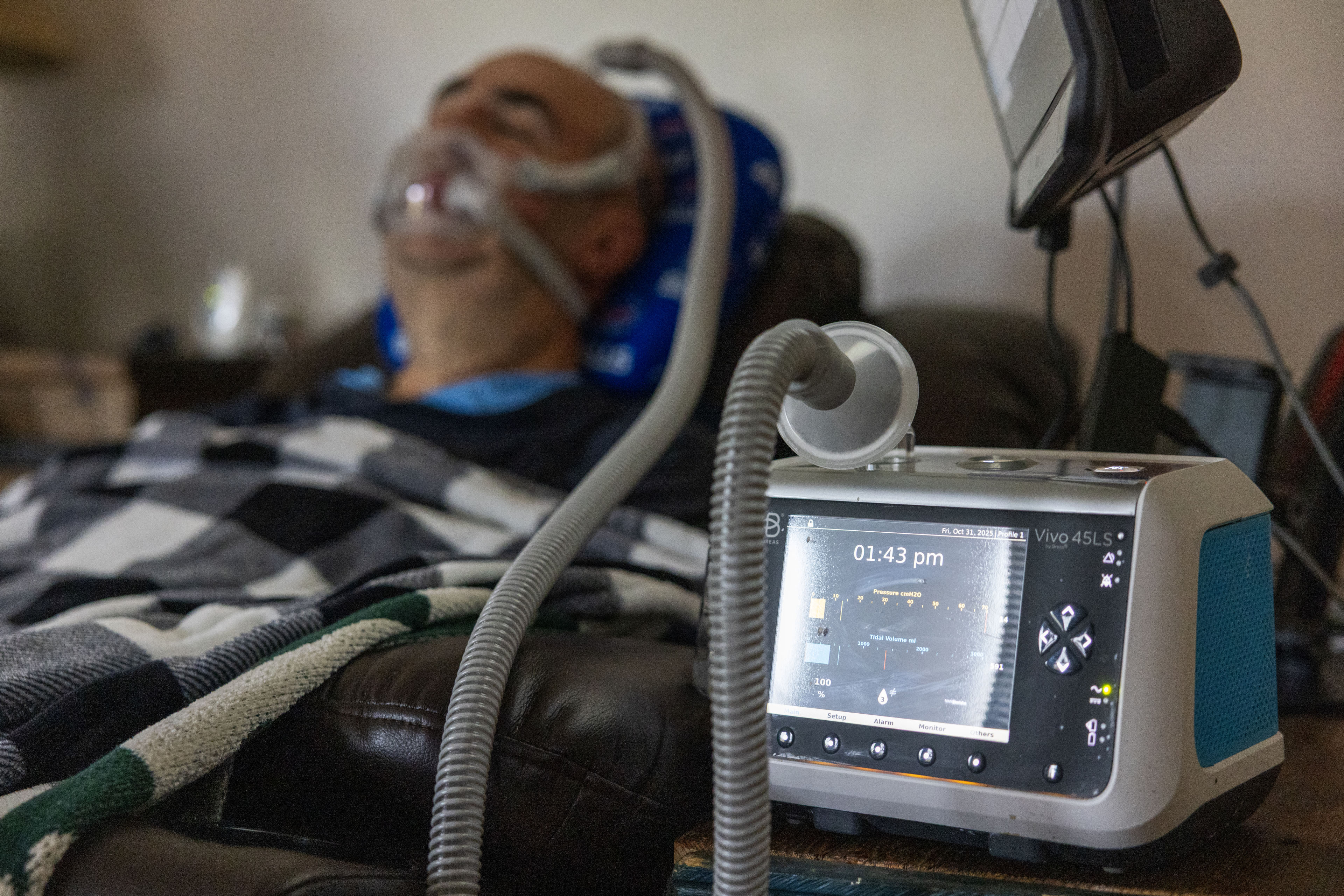
But some insurers have what physicians call “fail first” policies that won’t pay for ventilators unless the patient has already tried a respiratory assist device without success (as defined by the company). These simpler machines, the kind sleep apnea patients use, are not as effective in removing carbon dioxide as ventilators and lack safety features. Commonly known by the acronyms BiPAP or CPAP, they can cost $1,000 or more and need to be plugged into an electrical socket.
“It seems to be an expectation of insurance companies they should live the rest of their life attached to a wall outlet,” said Rehbein, the University of Rochester neurologist.
In November 2024, Derek’s insurer denied his physician’s request for a ventilator, writing that “you have not failed treatment” with the simpler device, according to the insurer’s letter, provided by his wife, Lesley McManus. By April, Derek’s breathing capacity had dropped to 60% of normal. Lesley said she worried he would suffocate overnight if his basic device stopped working, since it had no safety alert. “He couldn’t take the mask off, because he can’t move his hands,” she said.
The insurer denied a second request for a ventilator, reiterating that Derek had not shown the simpler machine hadn’t worked, according to another insurance letter. Derek, who is 56, appealed to an independent medical reviewer, who overturned the insurer’s decision and ordered it to provide a ventilator, according to a copy of the ruling. The doctor wrote that the machine’s alarm system and capacity to automatically clear away airway secretion by simulating a cough were “vital for patient safety” and would help protect Derek from developing pneumonia.
“This multi-faceted approach to respiratory care is essential for improving gas exchange, reducing the work of breathing, and ultimately enhancing the patient’s quality of life and extending survival,” the decision said.
Derek said that since he got the new machine, he’s breathing easier, literally and emotionally. “If I’m not breathing right, it will give it an alert, and it will let us know if I don’t have the mask on properly,” he said.
The McManus family requested KFF Health News not publish their insurer’s name, out of fear of repercussions.
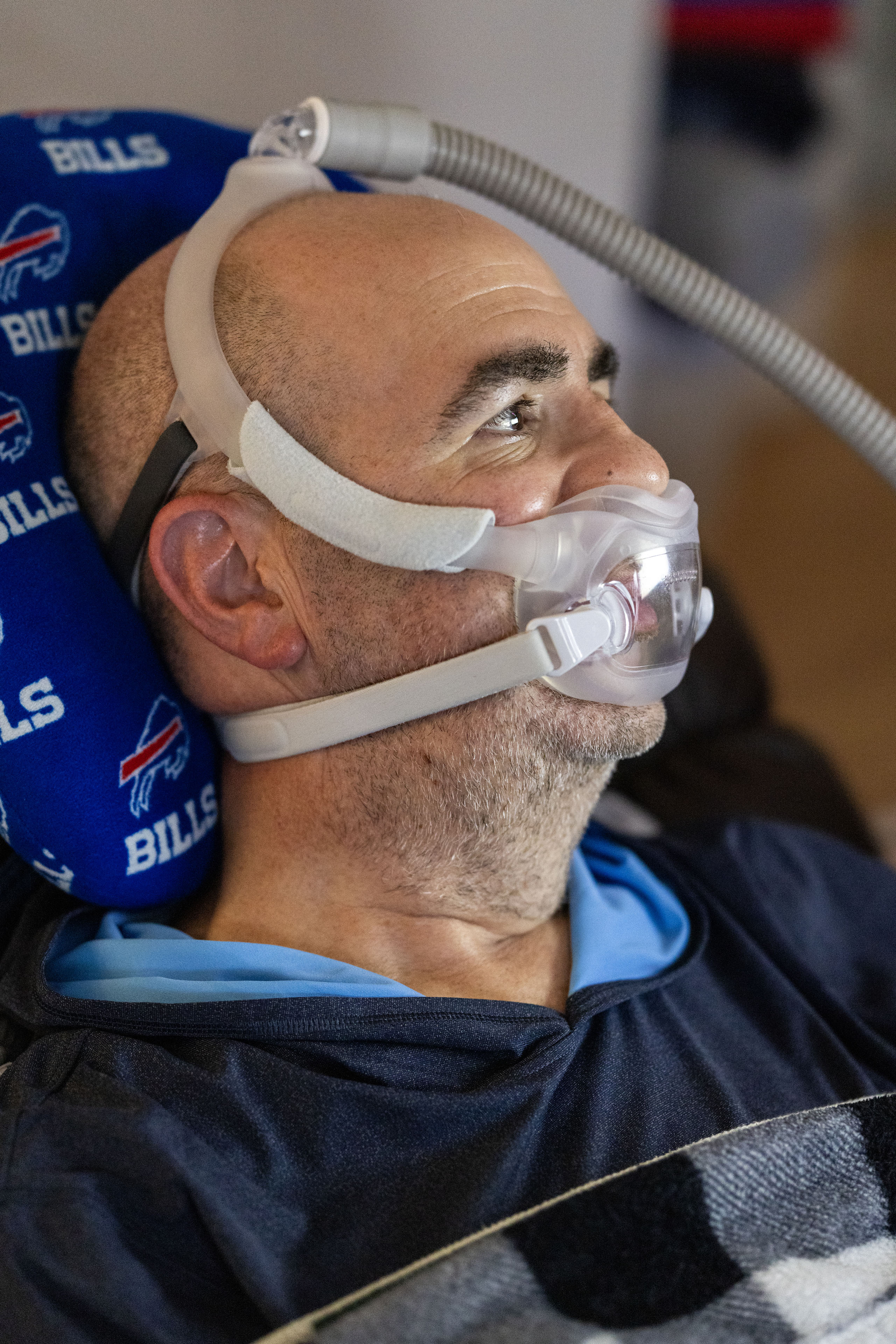
Insurance Rules
John Hansen-Flaschen, a pulmonologist who founded Penn Medicine’s program for home assisted ventilation, said some patients give up when an insurer denies their requests and don’t file appeals. “These are some of the most vulnerable people there are, and they don’t have energy to do this,” he said.
Doctors who treat patients with neuromuscular disorders said the most resistance to providing ventilators comes from some private Medicare Advantage plans, but they said it also has been an issue with some commercial policies.
Insurers dispute that they refuse ventilators for patients who need them. The written policy of Excellus BlueCross BlueShield, which Rehbein said was one of the companies that covers his patients, requires simpler breathing machines to have failed before patients can get the more sophisticated ventilator. After a KFF Health News inquiry, Excellus clarified its policy with a footnote saying it does consider mechanical ventilators as first-line therapy for certain situations, such as ALS, on a case-by-case basis.
UnitedHealthcare confirmed that some of its policies require that a less complex device be tried initially and found ineffective before a ventilator can be authorized. Aetna’s policy doesn’t mandate a stepped process and says it considers mechanical ventilators based on the severity of the condition and “where interruption or failure of respiratory support would lead to death,” with other patients eligible only for the simpler devices. Humana and Cigna did not respond to requests to provide their policies.
Chris Bond, a spokesperson for AHIP, the health insurance industry’s trade organization, said, “Health plans work to connect patients with safe, clinically appropriate care and welcome opportunities to work with policymakers and stakeholders across the health care system to continually improve access and precisely address any coverage-related issues.”
Melanie Lendnal, senior vice president for policy and advocacy at the ALS Association, said, “I haven’t met one person yet living with ALS, or a family member, who has not had to fight — really fight — to get a non-invasive ventilator.”
A Model in Massachusetts
In 2019, David Marion, a 36-year-old plumber, was hanging out with friends in Lowell, Massachusetts, when he tripped on the sidewalk and fractured his neck. The injury rendered him quadriplegic and paralyzed his abdominal and diaphragm muscles, requiring him to use a ventilator. Surgeons performed a tracheotomy, and over the next year and a half, Marion lived in two long-term acute care hospitals. “I didn’t get out of bed” at the second hospital, Marion, now 43, said in an interview.
His mother, Denise Valliere, who lives in New Hampshire, said she grew desperate trying to find a permanent home for him that was close enough that she could visit. “Some of those nursing homes are pretty sad places,” she said.
At the end of 2020, Marion’s luck turned. He was accepted by the Leonard Florence Center for Living in Chelsea, Massachusetts, which has created an alternative to the institutional life most nursing homes can offer people on ventilators. The center follows the Green House philosophy, with small residences each serving 10 people, with private bedrooms, a common living room, and outdoor space. Residents set their own schedules, including when and what to eat. The center has 10 residences in its building; six are dedicated to people dependent on ventilators, including those with ALS or MS.
The center’s respiratory therapists helped Marion get to the point where he didn’t need a feeding tube and didn’t require his ventilator for portions of the day. The center provided a portable ventilator attached to his wheelchair and a computer tablet that Marion operates with his mouth. It allows him to summon the elevator, open doors, go outside, and adjust his bed, window shades, temperature, and television settings. Other residents who can’t use their hands or mouths can operate the devices through a camera that captures eye movement.
“This gives back independence to people who never thought they’d have independence again,” said Barry Berman, the chief executive officer of Chelsea Jewish Lifecare, the nonprofit that owns the Leonard Florence Center. “There are alternatives. It doesn’t have to be the way that it is.”
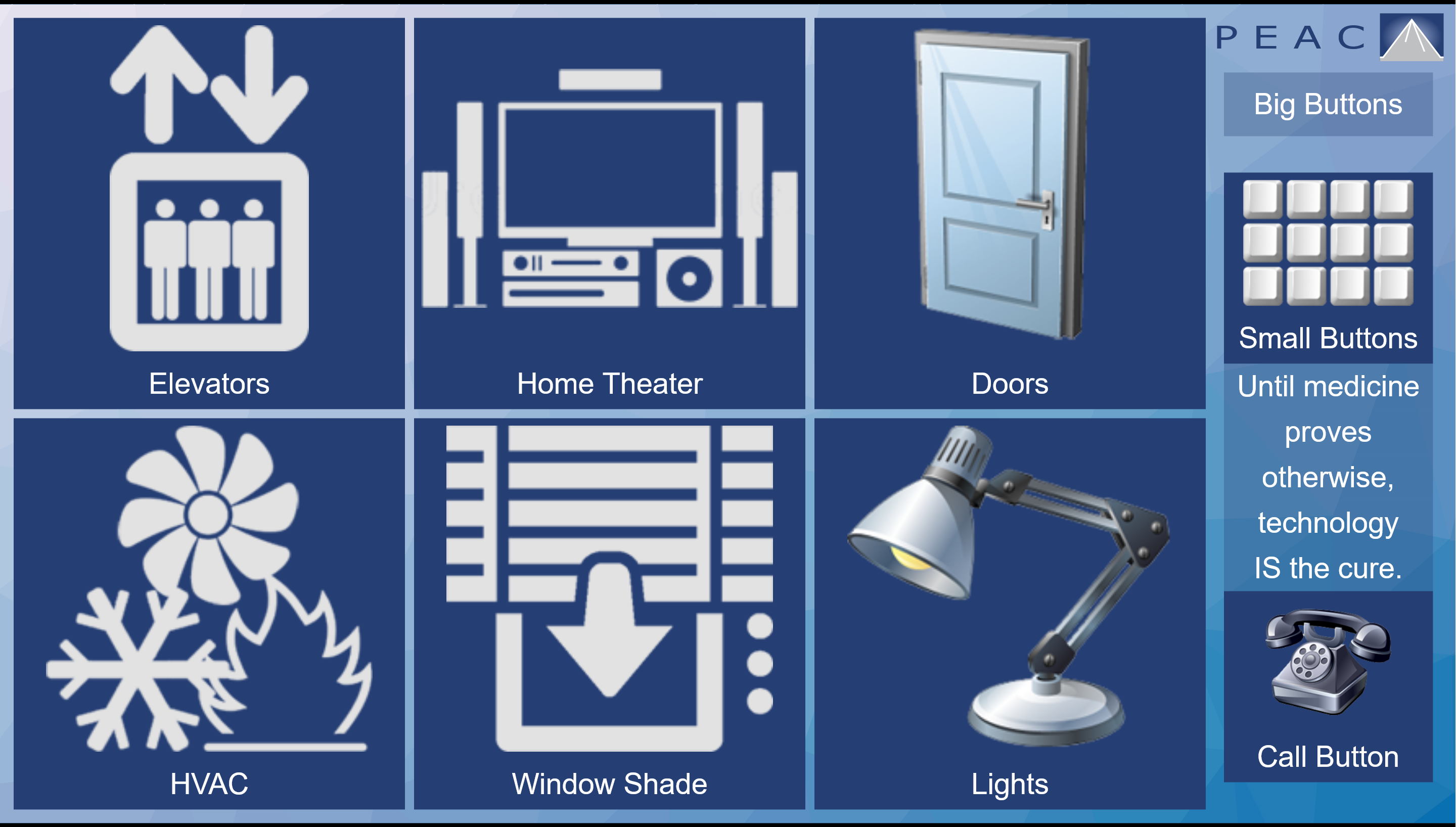
Most of the residents’ stays are paid for by Medicaid, which together with Medicare provides the bulk of the center’s revenue. Its finances are bolstered by the nonprofit’s endowment, something most nursing homes lack. Berman said that since the center opened in 2010, he has hosted dozens of visitors interested in replicating its model elsewhere in the country, but no one has.
Some states have licensed facilities that aren’t nursing homes to care for people on ventilators. In California, some people on ventilators live in “congregate living health facilities,” which are residential houses that provide 24-hour skilled nursing for the terminally ill, people who are catastrophically or severely disabled, or people who are mentally alert but physically disabled.
Patients often must pay privately because Medicaid managed care programs don’t include these facilities as a benefit, said Mariam Voskanyan, who is president of the state association representing congregate living facilities and owns one in Los Angeles. California’s Medi-Cal program is authorized to pay these kinds of facilities through its Home and Community-Based Alternatives waiver, but the program is at capacity and there is a waitlist of more than 5,000 people.
Researchers expect states will be under pressure to reduce or eliminate programs like these to make up for nearly $900 billion in coming Medicaid reductions, since the federal government does not require states to cover respiratory care for people on ventilators or nursing home alternatives.
Valliere, Marion’s mother, said she was baffled that there were not more places like Leonard Florence. “How can we be so behind in that kind of care and those kinds of facilities if we’re the best country in the world,” she asked. “Why is this?”


